There are a wide range of terms used to describe spinal conditions associated with back pain:
- Slipped disc
- Pinched nerve
- Bulging disc
- Ruptured disc
These names are used interchangeably, which can cause a lot of confusion, but all of them can irritate the nerve and cause back pain. Although these spine conditions can be very painful, many people recover after a few weeks or months with nonsurgical treatment.
Spinal Anatomy
The spine is comprised of small bones called vertebrae. These are stacked on top of each other and form the natural curves in your spine. The vertebrae provide a protective layer for the spinal cord and nerves. Between each set of vertebrae, there are small, round discs that act as a cushion between the vertebrae. Each disc has a jelly-like center (nucleus) that is surrounded by a tough outer ring (annulus).
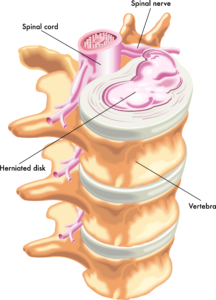
What is a Herniated Disc?
A herniated disc, also known as a slipped or ruptured disc, is a medical condition that occurs when the soft inner core of a spinal disc pushes through a tear in the tougher outer layer. These discs are located between the vertebrae (bones) of the spine and act as shock absorbers, providing cushioning and flexibility to the spine.
When a disc herniates, it can put pressure on nearby nerves or the spinal cord, causing pain, weakness, or numbness in the affected area which is known as lumbar radiculopathy. The specific symptoms and severity of a herniated disc depend on the location of the herniation and the extent of the pressure on the nerves.
Herniated discs most commonly occur in the lower back (lumbar spine) or the neck (cervical spine). Common causes of herniated discs include age-related wear and tear, sudden trauma, or activities that involve repetitive or heavy lifting.
Bulging vs Herniated Disc
A bulging disc and a herniated disc are related spinal conditions, but there are important distinctions between them:
- Bulging Disc:
- A bulging disc occurs when the disc’s outer layer (annulus fibrosus) weakens or degenerates, causing the disc to extend beyond its normal boundaries. This means that the disc is still intact, but it has expanded or protruded outward.
- The bulging disc may press against nearby nerves or the spinal cord, potentially causing pain, tingling, or weakness, but the outer layer of the disc is still intact.
- It is generally considered a less severe condition compared to a herniated disc.
- Herniated Disc (or Ruptured or Slipped Disc):
- A herniated disc is a more advanced stage of degenerative disc disease. It occurs when the soft inner core (nucleus pulposus) of the disc actually ruptures through a tear or hole in the outer layer (annulus fibrosus) of the disc.
- In a herniated disc, the inner material of the disc is exposed, and it can protrude out into the spinal canal, potentially impinging on nerves or the spinal cord.
- This condition is often associated with more significant symptoms, including severe pain, numbness, tingling, and muscle weakness.
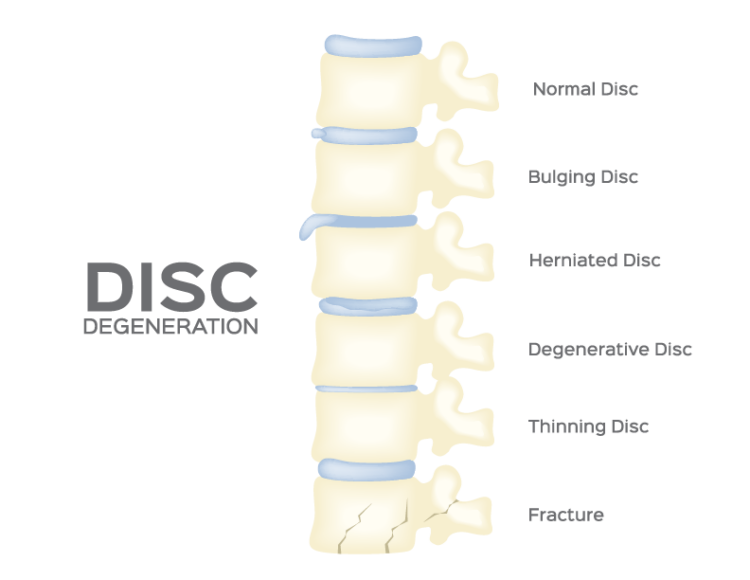
The key difference lies in the integrity of the disc’s outer layer. In a bulging disc, the outer layer is still intact but has extended beyond its usual boundary. In a herniated disc, there’s an actual rupture or tear in the outer layer, allowing the inner material to protrude out.
Both conditions can cause discomfort and potentially lead to nerve compression or irritation, but a herniated disc is generally considered more severe due to the direct exposure of the inner disc material.
How Disc conditions are diagnosed
Disc conditions are diagnosed through a process that involves a thorough medical history and physical examination, including a neurological assessment. Imaging studies like X-rays, MRI, and CT scans provide detailed views of the spine, highlighting issues such as herniated or bulging discs, nerve compression, and other spinal abnormalities. Additional tests like EMG, NCS, and discography may be used for more specific evaluations.
How Disc conditions are treated
Treatment options for both a bulging disc or herniated disc may include rest, physical therapy, pain management, and in some cases, surgery, depending on the severity and individual circumstances. Consulting a healthcare professional is crucial for proper diagnosis and treatment. It’s important to note that not all herniated discs cause symptoms, and some people may have one without even knowing it. If you suspect you have a herniated disc or are experiencing back or neck pain, it’s important to consult a healthcare professional for proper evaluation and guidance.
If conservative treatments prove ineffective for pain relief, your neurosurgeon might suggest a lumbar microdiscectomy, a common surgical solution for alleviating back pain caused by herniated or bulging discs. This procedure entails the removal of the herniated portion of the disc and any fragments that exert pressure on the spinal nerve. A lumbar microdiscectomy is an outpatient surgery, allowing you to return home the same day, without an overnight hospital stay. Following the procedure, patients will start physical therapy and learn core-strengthening exercises. A minimum of three months is required for recovery before resuming regular activities. Given the presence of a hole in the annulus in the case of a herniated disc, its original strength will not be fully restored. It’s essential to allow ample time for healing and avoid exerting excessive stress on it too soon.
What is a pinched nerve?
A pinched nerve, medically known as nerve compression or impingement, occurs when excessive pressure is applied to a nerve by surrounding tissues such as bones, cartilage, muscles, or tendons. This pressure disrupts the nerve’s normal function, leading to symptoms like pain, tingling, numbness, or weakness in the area that the nerve serves.
Pinched nerves can happen anywhere in the body, but they are most commonly observed in the spinal column (such as in cases of disc herniation or spinal stenosis) or in areas where nerves pass through narrow or confined spaces, like the wrists (carpal tunnel syndrome) or elbows (cubital tunnel syndrome).
What is the treatment for a pinched nerve?
Treatment for a pinched nerve may involve rest, physical therapy, non-steroidal anti-inflammatory drugs, and sometimes, in severe cases, surgery. The specific approach will depend on the location and severity of the pinched nerve and the individual patient’s condition. If left untreated, a pinched nerve can lead to chronic pain and potentially long-term nerve damage, so it’s important to seek medical attention if you suspect you have a pinched nerve.
What is the difference between a pinched nerve and a herniated disc?
A pinched nerve and a herniated disc are related but distinct conditions:
- Pinched Nerve:
- A pinched nerve, also known as nerve compression or impingement, occurs when excessive pressure is applied to a nerve by surrounding tissues. This pressure disrupts the nerve’s normal function, leading to symptoms like pain, tingling, numbness, or weakness in the area that the nerve serves.
- Pinched nerves can happen anywhere in the body but are commonly observed in areas where nerves pass through narrow or confined spaces, like the spine (spinal stenosis) or areas like the wrists (carpal tunnel syndrome) and elbows (cubital tunnel syndrome).
- Herniated Disc:
- A herniated disc, on the other hand, specifically refers to a condition where the soft inner core of a spinal disc protrudes through a tear in the tougher outer layer. These discs are located between the vertebrae of the spine and act as shock absorbers.
- When a disc herniates, it can put pressure on nearby nerves or the spinal cord, causing pain, weakness, or numbness in the affected area.
In summary, while a herniated disc can cause a pinched nerve if it presses against nearby nerves, a pinched nerve can occur independently due to various reasons like pressure from surrounding tissues or conditions like carpal tunnel syndrome. The distinction lies in the underlying cause: a herniated disc involves a specific issue with the intervertebral discs in the spine, while a pinched nerve can arise from various factors affecting nerves throughout the body. It’s important to note that these conditions can sometimes co-occur, further complicating an accurate diagnosis and treatment. Consulting a healthcare professional is crucial for proper evaluation and treatment.
Stay informed about upcoming webinars and events, and gain valuable insights on leading a healthy, pain-free life from our experts by subscribing to our monthly newsletter. Click the button below to join!





